

COVID-19 Financial Recovery: Leverage Your Workforce to Prepare for the Future
By Frances Roelfsema, MBA
Moss Adams
By Bob Van Gelder, RN, MBA
Moss Adams
Original Publish Date: April 6, 2021
Health care leaders endured a challenging 12 months following the outbreak of the COVID-19 pandemic, potentially the most trying of their careers. As the other side of the pandemic approaches, hospitals that survived its financial toll can begin to evaluate how to recover and improve their financial performance as well as prepare for their organization’s long-term financial stability.
While hospitals in different regions will continue to experience varying consequences from the pandemic, your organization can start developing thoughtfully crafted plans to position for a more stable world, now.
Below, we outline strategies for the future and explore how focusing on your workforce can help you plan for what’s next.
What Labor Factors Should Hospitals Keep in Mind?
Labor costs typically make up 50%–55% of a hospital’s operating expense structure; focusing on labor expense should be a top priority to position your organization to meet current and future needs.
Fortunately, improving labor productivity doesn’t necessarily equate to reducing your workforce.
It does, however, require a serious analysis of financial performance; labor costs; productivity benchmarking against peer hospitals; and thoughtfully designing, communicating, and deploying performance improvement tactics throughout your organization.
What Pitfalls Should Hospitals Avoid While Planning for Recovery?
Common mistakes can arise while executing a large financial improvement initiative or turnaround project, and these mistakes strongly correlate with project failure or significant underperformance.
Common Leadership Pitfalls
The following gaps in leadership oversight can significantly hinder your initiative’s potential:
- Lack of visible leadership and failure to act as passionate project champions
- Underinvestment in project management, communications strategy, and resources
- Failure to acknowledge management team weaknesses and address low performers upfront
- Inability to hold management accountable for failing to meet their respective targets
- Lack of engagement with key stakeholders in all phases of the project
- Failure to evaluate and address so-called sacred cows which have a negative bottom-line impact
- Plans for across the board reductions to simplify the process, which are frequently counterproductive for well-run departments and unsustainable
If your leadership team can commit to avoiding these common pitfalls, embarking on a plan to improve your labor operating expenses can be easier to implement.
Operational Strategies to Drive Success
Here are some key take-aways to help drive your success:
- Commit to taking decisive action
- Use a structured, systematic approach
- Avoid pursuing solutions alone and recognize help is available
What Will Recovery Planning Look Like for an Organization?
Planning should take place over three phases.
Phase One: Conduct a Current Assessment
The first step to improving performance is to assess your current state. Current performance versus budget expectations is a critical indicator for your organization’s financial health.
Benchmarking performance against regional and volume-based peers is another often overlooked but vital assessment. Publicly available data, as well as proprietary databases from various organizations, can help provide insights into how your organization performs and what may be reasonably attainable through improvement initiatives.
Perform High-Level Benchmarking
In the scenario below, a hospital performs in the lowest quartile compared to its peers.
Usually, failing to correct this situation comes with negative consequences, and thus the status quo likely isn’t sustainable.
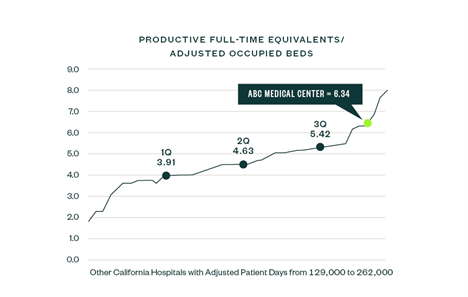
Identify Department-Level Opportunities
First, identify areas that warrant further attention by engaging with department directors and managers as part of an initial performance assessment.
Establishing trust with department leaders requires asking the right questions to understand all the variables that may impact the poor performance results.
Important questions to ask include:
- How did COVID-19 impact your department?
- What normal seasonality patterns affect your volumes?
- Is there anything unusual about your department that makes it different from similar departments at other hospitals?
- Are there any physical limitations to your department that affect your ability to deliver quality care efficiently?
- How accurate are your productivity reports? Are there patients or procedures for which you don’t get so-called productivity clicks?
- Do any staff show up in your cost center who don’t belong there? Do those reports accurately reflect employees who work for multiple cost centers?
- What are your staffing challenges? Do you need to routinely use premium pay, travelers, or agency personnel to fulfill your staffing needs? Does your facility have an effective float pool to help fill gaps in your daily staffing?
- What is your staff turnover rate? Do you have trouble recruiting and filling vacancies?
Phase Two: Identify Solutions
Communicate the Vision
As you evaluate opportunities and your labor efficiencies, engage in robust dialogue with key stakeholders to garner support for the performance improvement vision.
Commit to labor targets with a clear understanding of the benefits. Targets should then be assigned to individual executives, directors, and managers based on the results of the phase-one assessment.
Support and Empower Department Managers
Follow these steps to support your managers:
- Support and empower managers. Empower the department managers to develop appropriate solutions to the challenge they’ve been presented. Provide support to managers with large targets or those with less apparent strengths to creatively close the gaps throughout the process.
- Connect with an outside consultant. Consider leveraging consultants with expertise in labor cost management to help managers examine all the key levers, including ascertaining managers’ own ideas and vetting and quantifying the impacts.
- Provide industry insight. Share relevant industry best practices that might help your organization.
- Base decisions on data. Perform detailed modeling and other analytics to help identify opportunities.
In addition to supporting managers as they develop needed solutions and turn them into action plans for meeting their targets, a good leader will:
- Provide education and mentoring
- Share tools to allow managers to more effectively control their labor costs going forward
Phase Three: Implement Your Plan
Implementation is typically the most challenging phase. Successful leaders will provide support, monitor progress, remove barriers, verify communication continues, and hold people accountable for achieving their results.
The initiative and the business imperative need to remain highly visible to keep people engaged and moving in the same direction.
As this phase concludes, it’s important to develop plans to continue monitoring all impacts and address any slippage to hold the gains.
Success Story Examples
Hospitals that have successfully utilized these strategies include:
- A 350-bed teaching hospital in Ohio that identified over $9 million in labor cost reductions versus a target of $7.9 million
- A 300-bed community hospital in Central California exceeded its targeted labor cost reduction of $6.6 million with over $9.2 million in improvements identified and approved for implementation
- A 150-bed community hospital in Northern California that identified over $11.2 million in performance improvements versus a target of $9.5 million
What Next Steps Can a Hospital Take?
Assessing results and identifying performance gaps or opportunities for improvement may not only be warranted, but also critical for the hospital’s overall performance.
Action is required; leadership needs to engage stakeholders, including physicians, nurses and staff to craft a careful, detailed path forward. This involves the following actions:
- Fully determining the business imperative and target setting
- Creating needed project infrastructure
- Developing a robust communication plan to deploy throughout the organization
Seek Guidance for Your Strategies
Organizations that choose to create complex improvement initiatives on their own could reach sustainable results much more slowly, or they may fail to focus on the right opportunities and avoid less productive options.
Working with experienced professionals can help you better develop the following key features
- A goal-setting process tightly tethered to your situation and business imperative
- A structured, proven approach grounded in rigorous and actionable analytics to identify opportunities and facilitate solutions
- A collaborative style tailored to your situation and committed to maintaining quality, safety, and satisfaction
- Experience and expertise across all areas of hospital operations
- Committed resources with expertise in project management, change management, and communications
We’re Here to Help
To start preparing your organization for COVID-19 recovery or learn more about these strategies, please contact your Moss Adams professional.
Frances Roelfsema, MBA, has more than 35 years of experience in health care operations and consulting. She has held senior positions at large integrated health systems and health care consulting firms. She can be reached at 628-208-8320 or frances.roelfsema@mossadams.com.
Bob Van Gelder, MBA, RN has more than 40 years of health care experience in health care. He specializes in strategic planning, budget management, clinical operations assessments, clinical staffing analysis, and more. He can be reached at (916) 503-8276 or bob.vangelder@mossadams.com.
Assurance, tax, and consulting offered through Moss Adams LLP. Investment advisory services offered through Moss Adams Wealth Advisors LLC.